
Learning about what works in urgent community response
The initial report from the national urgent community response (UCR) evaluation, along with an economic modelling tool to help service providers and systems understand the impact of UCR, is now available.

Diagnosing harms?
All medicines are poisons. Everything that cures could kill if administered in the wrong doses, to the wrong people, at the wrong times, in the wrong ways.
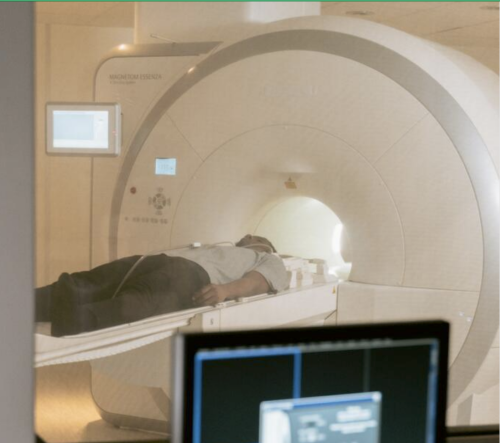
How is growth in diagnostic testing affecting the hospital system?
Diagnostic services, such as medical imaging, endoscopy, and pathology, have grown substantially in recent years and at a faster rate than most other healthcare services. Increased diagnostic testing brings benefits to patients, but rapid growth of this service area within a complex, adaptive system such as the NHS is likely to have had unintended consequences. Midlands ICBs wanted to understand the impact of diagnostic growth on hospital services.

The NHS as an anchor institution: addressing fuel poverty
The number of households in fuel poverty in Staffordshire and Stoke-on-Trent (SSoT) is higher than the national average. As anchor institutions, NHS organisations can use their assets to influence the health and wellbeing of their local communities. The Strategy Unit was asked by the Midlands NHS Greening Board to evaluate a cross-sector initiative in SSoT to help alleviate fuel poverty using savings generated through solar panels on NHS buildings. The project is called Keep Warm, Keep Well.

Urgent Community Response – What Works?
The Strategy Unit, with our partners Ipsos, has been commissioned by NHS England and NHS Improvement (NHSEI) to provide a long-term national evaluation of the Urgent Community Response programme rolled-out across England. The programme aims to shift resources to home and community-based services as part of the NHS commitment to providing the right care, to the right people, at the right time. And there are a range of outputs from the early work that provide learning for local systems as they develop their services.

‘Developing your ICS Intelligence Functions’: A Free Webinar Series
What is an ‘Intelligence Function’? What value can they add to decision making? How can they be configured and who needs to be involved? What lessons can be drawn from current practice?

Evaluation of Building the Right Support: Final Reports
Building the Right Support was a national plan to provide better support to people with a learning disability or autism.

Advancing the analytical capability of the NHS and its ICS partners
The Strategy Unit were asked by the Strategy and Development Team in the Directorate of the Chief Data and Analytics Officer, NHSE/I, to make recommendations for advancing analytical capability across the health and care workforce.

Strategy Unit devises a new method for classifying outpatient appointments
The number of outpatient attendances in England is now approaching 100 million each year.

Inequities in children and young people’s mental health services
Good mental health during early years and childhood has a great bearing on health throughout life.

Less noise and more light: using criteria-driven analysis to tackle inequalities
Reducing health inequality is a long-standing aim of health policy. Yet the gap between policy aim and population outcome has grown in recent years: on most measures health inequalities have got worse.

Learning from lockdown: support for people experiencing homelessness
There are few clearer measures of societal health than homelessness.
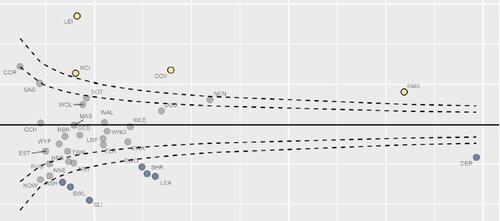
Equity and Cost Growth in Specialised Services
NHS specialised services provide care for people with complex or rare medical conditions.

A free guide to support high quality evaluation in the NHS
The Strategy Unit issues free guide to evaluation principles and practice

Evaluating Artificial Intelligence: a significant new win
The Strategy Unit, the Health Economics Unit and Leicester Clinical Trials Unit have been announced as evaluation partners to support success in the Artificial Intelligence (AI) in Health and Care Awards.

How can we learn from changes in practice under COVID-19
During the COVID-19 pandemic we have seen rapid changes in ways of working.
Primary and Community Qualitative Insights
The COVID-19 response required rapid change and innovation across health and care.
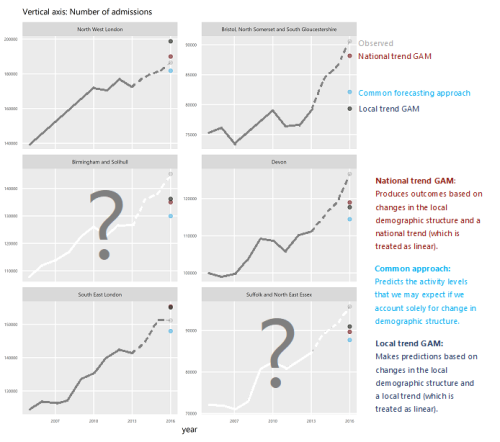
How will we know if Integrated Care Systems reduce demand for urgent care?
The implications of a blended payment system are far reaching: Decisions about planned activity levels will determine the total funding envelope for urgent care within a system and will influence the behaviour of healthcare providers and the services they deliver to patients.

