 Strategy Unit information
Strategy Unit information
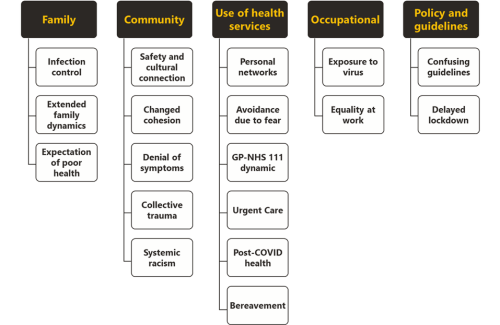
We don’t just need to hear ‘you are more affected’ - what’s the action?
The experience of minority ethnic people symptomatic for COVID-19 in the first UK wave of the pandemic.
 Better use of analysis | Elective care | Emergency care | Inequalities | Primary, community and social care services | Public health and prevention
Better use of analysis | Elective care | Emergency care | Inequalities | Primary, community and social care services | Public health and prevention
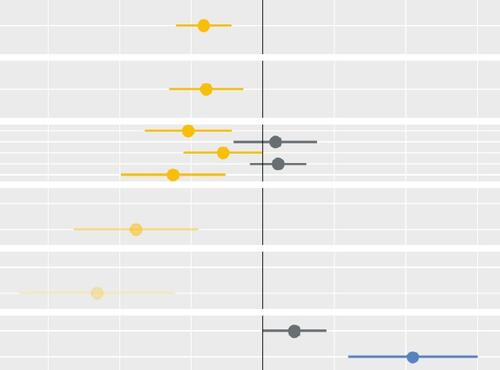
Less noise and more light: using criteria-driven analysis to tackle inequalities
Reducing health inequality is a long-standing aim of health policy. Yet the gap between policy aim and population outcome has grown in recent years: on most measures health inequalities have got worse.
 Elective care | Inequalities | Policy | Primary, community and social care services
Elective care | Inequalities | Policy | Primary, community and social care services
Socio-economic inequalities in access to planned hospital care: causes and consequences
Tacking inequalities in health is a long-standing NHS policy objective. Variation in the experiences and outcomes of different communities during the COVID-19 pandemic served to bring this issue back into focus.
 Elective care | Emergency care | Finance and payments | Policy | Primary, community and social care services
Elective care | Emergency care | Finance and payments | Policy | Primary, community and social care services
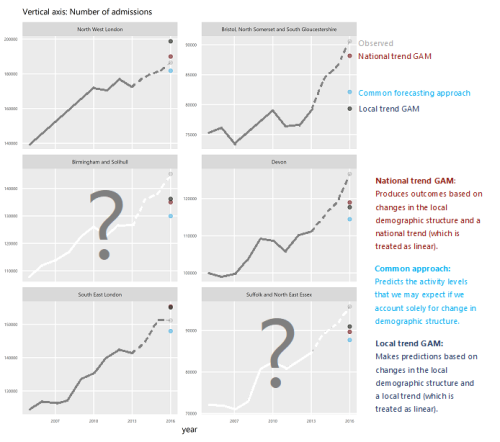
How will we know if Integrated Care Systems reduce demand for urgent care?
The implications of a blended payment system are far reaching: Decisions about planned activity levels will determine the total funding envelope for urgent care within a system and will influence the behaviour of healthcare providers and the services they deliver to patients.