
“Champion, challenge, collaborate.”
Being commissioned by the Mayor of London to produce independent reviews of proposals for major service change, affecting Londoners, perfectly aligns with our commitment to help the health and care system make better decisions and ultimately achieve benefits for population health and wellbeing.
Socio-economic inequalities in coronary heart disease
There are substantial differences in mortality rates from cardiovascular disease between socio-economic groups. Our new tool provides an overview, for ICBs, of the points on the care pathway where inequalities emerge and are amplified
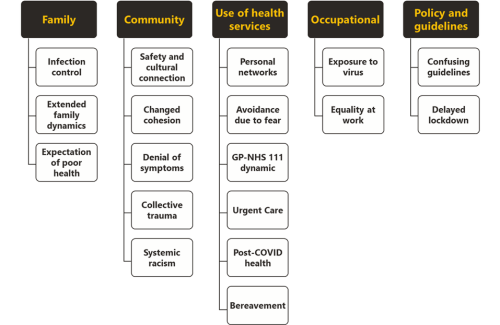
We don’t just need to hear ‘you are more affected’ - what’s the action?
The experience of minority ethnic people symptomatic for COVID-19 in the first UK wave of the pandemic.

Less noise and more light: using criteria-driven analysis to tackle inequalities
Reducing health inequality is a long-standing aim of health policy. Yet the gap between policy aim and population outcome has grown in recent years: on most measures health inequalities have got worse.
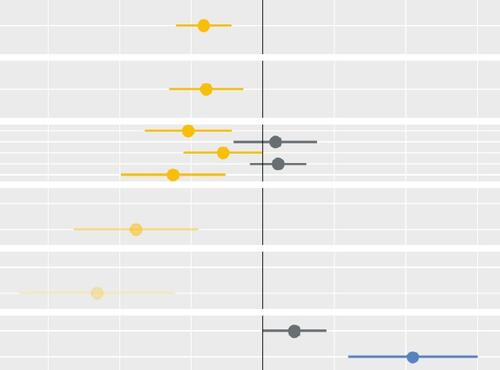
Socio-economic inequalities in access to planned hospital care: causes and consequences
Tacking inequalities in health is a long-standing NHS policy objective. Variation in the experiences and outcomes of different communities during the COVID-19 pandemic served to bring this issue back into focus.
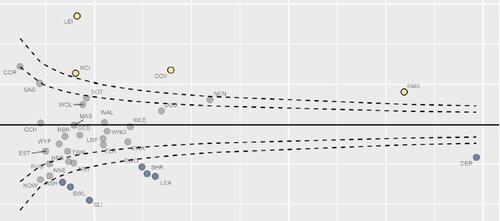
Equity and Cost Growth in Specialised Services
NHS specialised services provide care for people with complex or rare medical conditions.

Socio-economic and environmental impact of Herefordshire and Worcestershire STP
Anchor institutions are large, typically non-profit, public sector organisations whose long-term sustaina

Accessibility of perinatal mental health services for women from Ethnic Minority groups
Barriers to accessing mental health care during pregnancy and the first postnatal year (perinatal period) seem to be greater for ethnic minority women.
Outcomes based commissioning: A framework for local decision making
This local decision-making framework aims to empower systems as they look to design new contracting approaches aimed at improving outcomes.

Key opportunities for eye health and well being
Eye health and sight loss services have historically had a lower profile in service provision compared to many other specialities. There is a view that the importance of eye health has been underrepresented in many Sustainability and Transformation Partnership (STP) plans.
Measuring what matters in systems – A call for person-centred intelligence
The Strategy Unit and Ipsos MORI launch guide to implementing Person-Centred Intelligence.
Lessons, Evaluation and Learning from the Dudley MCP
Learning from Dudley MCP
The Potential Economic Impact of Virtual Outpatient Appointments in the West Midlands: A scoping study
The Strategy Unit was recently approached to examine the case for a shift from traditional outpatient services to the use of virtual a
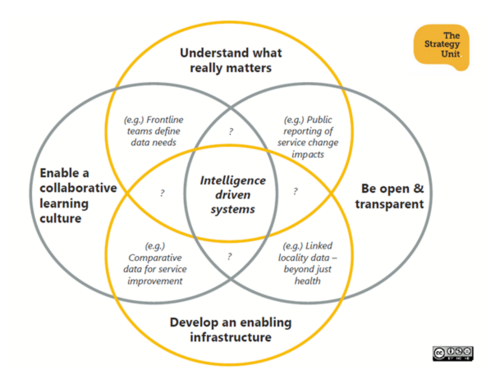
Intelligence-driven health and care: phase two
Following on from the Design Summit in
Evaluation of the Dudley New Care Models Programme
The Strategy Unit led the evaluation of the Dudley Vanguard programme. This is the final system-wide report from that work.
Evaluation of the Dudley New Care Models Programme
This is the final system-wide report from the evaluation.

Intelligence-driven healthcare: what should the future look like?
Find out about our recent summit on intelligence to drive improvement in healthcare and comment on our working design principles.
Dudley System Performance Report
In order to help Dudley's Partnership Board track progress towards high level goals, this report presents a series of performance measures for Dudl
Understanding future maternity demand and activity using collaborative modelling methods
The Strategy Unit approach to demand and activity modelling has been developed, refined and extensively tested over many years in a variety of heal
Innovation In Dudley: The Enabling Practice To Improve And Change Programme (Epic)
The Strategy Unit has been working with GP practices in Dudley for the last three years to support service improvement in Primary Care.